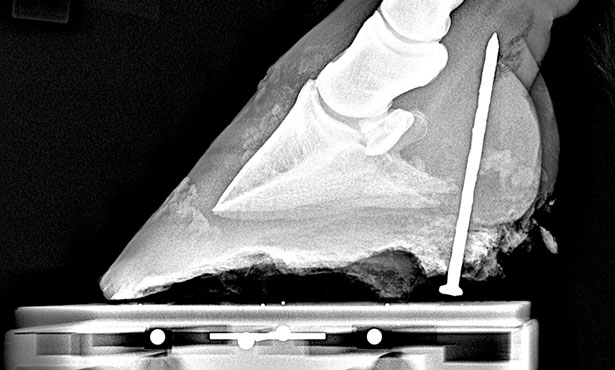
Imagine your horse coming in from the field toe-touching lame, just hours after you turned him out, perfectly sound. You do not see any wounds on the limb, but there is a mild amount of heat and swelling present from the hoof to fetlock region. You lift the hoof to inspect for an abscess, and much to your horror and surprise you discover a nail head protruding from the bottom of your horse’s hoof!
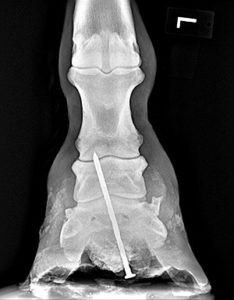
What do you do?
A) Remove the nail immediately, soak the hoof, and administer a tetanus vaccine
B) Remove the nail immediately and call your veterinarian
C) Leave the nail in the hoof and call your veterinarian
Answer: C
Nails should ONLY be removed by your veterinarian after they have evaluated the nail’s location and determined the necessity of radiographs.
It is a horrible sinking feeling to see your horse come in from the field suddenly lame. As horse owners, our immediate response is often to search for the source of the lameness and do our best to remedy it. This information can be very valuable to your veterinarian when you call, however, nails or other objects that have punctured the bottom of the hoof, sometimes called “street nails,” require careful veterinary inspection and often radiographs.
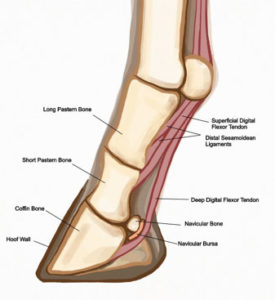
Hoof Anatomy
While farriers routinely place nails through the non-sensitive hoof wall and white line that form the capsule of the hoof, the inside of the hoof capsule is home to many important structures. Those structures include bones, tendons, ligaments, and joints, all of which can be difficult to treat for infection caused by a puncture wound. In addition, the spongey nature of the sole, frog, and heel can make identifying the puncture tract very difficult once the inciting cause, such as a nail, has been removed.
This is why it is important to leave the nail in place so that your veterinarian can evaluate the location of the object puncturing the hoof and perform radiographs to determine if there is any involvement with the deeper structures of the hoof.
Treatment
If it is determined that the penetrating object does not affect any important structures, the object is removed and the wound is treated similarly to a hoof abscess. This may include soaking the hoof and applying bandages to prevent further contamination. Your veterinarian may choose to open the area around the tract to facilitate drainage and may prescribe antibiotics and a tetanus vaccine.
 If it is determined that the penetrating object does affect important structures within the hoof, more aggressive management will need to be taken. This often includes referral to a hospital where regional limb perfusions and surgery may be necessary.
If it is determined that the penetrating object does affect important structures within the hoof, more aggressive management will need to be taken. This often includes referral to a hospital where regional limb perfusions and surgery may be necessary.
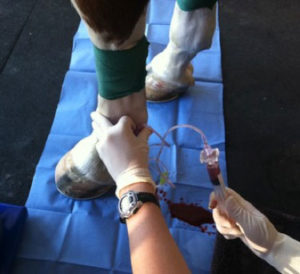
Regional limb perfusion (RLP) is a procedure that increases antibiotic concentration in the lower limb as oral or injectable antibiotics that go through the entire body, often not reaching high enough concentrations to be effective deep in the lower limb structures. This procedure is performed under standing sedation where a tourniquet is placed just above or below the knee and antibiotics are administered intravenously into the limb. The tourniquet holds the antibiotics in the distal limb and is left in place up to 40 minutes. This procedure may need to be performed multiple times over several days.
Surgery under general anesthesia may also be required to explore the path of the wound and to lavage or flush any joints or tendon sheaths (tubular structures the tendons slide through) that may have been contaminated with bacteria.
Outcome
Ultimately, time is key, and the sooner puncture wounds to the hoof receive veterinary attention, the better the outcome. Puncture wounds that do not affect any of the important structures within the hoof often heal nicely with appropriate veterinary intervention. However, when puncture wounds involve the deeper structures within the hoof, the prognosis varies and greatly depends on timely veterinary intervention and aggressive treatment. Unfortunately, some puncture wounds to the hoof can result in irreparable damage. Ultimately, if there is concern for involvement of bone, tendons, ligaments, or joints, surgical exploration is warranted to confirm the radiographic findings and provide the best treatment possible.