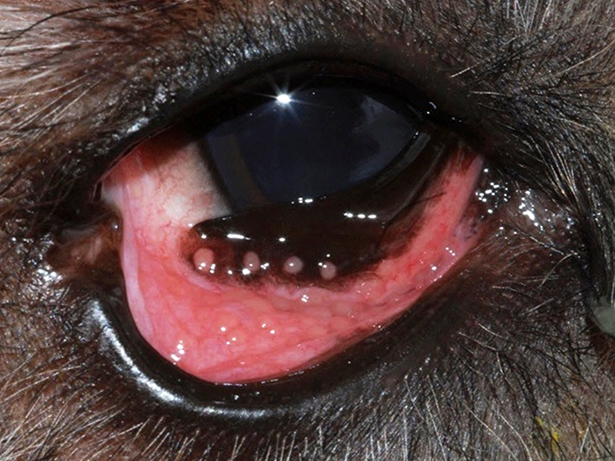
Multiple pink, raised follicles can be seen on the anterior third eyelid and along the ventral palpebral conjunctiva in this dog, giving it a cobblestone-like appearance.
We all know that conjunctival redness, or hyperemia, has many causes. Not all redness is cause for alarm, however, as it can result simply from anxiety or excitement. That being said, conjunctival hyperemia can also indicate something more serious, such as glaucoma or uveitis. Therefore, any persistent conjunctival hyperemia, especially when combined with discomfort or vision changes, should be investigated. As causes and treatments vary, a systematic approach to conjunctival hyperemia is imperative.
Clinical signs attributable to conjunctivitis include conjunctival hyperemia, swelling (chemosis), and ocular discharge. All dogs presenting with these signs should undergo complete ophthalmic examination to identify the source. In addition, Schirmer tear testing, fluorescein stain application, and tonometry should be performed to rule out dry eye, corneal ulceration, and glaucoma, respectively.

It is important in all cases to rule out concurrent corneal or intraocular disease. Delaying treatment for these conditions could result in permanent damage to the eye and possibly loss of vision. Systemic disease such as distemper can also cause conjunctivitis. Therefore, a complete physical examination should also be performed.
Once you have verified the patient has simple conjunctivitis and not conjunctival inflammation secondary to other ocular or systemic disease, the focus should turn to identifying an etiology. Unlike the condition in humans and cats, conjunctivitis in dogs is rarely caused by surface infection, and topical antibiotic therapy is rarely indicated. Rather, allergies and environmental irritation are more common etiolgies.
Foreign material can hide or embed itself deep within the conjunctival fornices and/or behind the third eyelid and should be removed, if found on examination. Allergic conjunctivitis may be accompanied by follicle formations, which appear as multiple 1- to 3-mm raised bumps on the conjunctiva. Follicles are normally found on the posterior surface of the third eyelid but should not be present elsewhere. Any focal swellings or masses should be sampled by scraping or biopsy to rule out neoplasia and parasites.
Small pieces of conjunctiva can typically be snipped away without need for site repair. Remember to grasp tissue gently and thereby minimize crush artifact. Extreme care should be taken when sampling the third eyelid so as not to expose the underlying cartilage.
Mild conjunctivitis can occur secondary to canine herpesvirus but appears to be self-limiting. Antiviral therapy is not necessary nor recommended in dogs. Parasitic conjunctivitis is rare in dogs, with most cases occurring secondary to Onchocerca lupi. Canine ocular onchocerciasis is most commonly reported in the southwestern United States and California and typically causes subconjunctival mass formation. Biopsy of these masses reveals parasitic larvae. Treatment strategies vary and cure can be difficult to achieve.
Follicular conjunctivitis is common in dogs less than 2 years of age and is thought to occur secondary to environmental irritation. Most dogs will grow out of this condition as they build immune tolerance. Follicular conjunctivitis can also occur in older dogs or those with deep orbits or lower eyelid ectropion. In these cases, pollen, dust, and debris can settle in the lower conjunctival fornix and persist there due to patient conformation.
Treatment of follicular conjunctivitis focuses on reducing or eliminating the stimulus. A conservative approach should be used at first, consisting of rinsing the eyes once to twice daily with eye irrigation solution. Topical ophthalmic lubricating gel can also be applied as needed, such as prior to taking the dog on a walk, to act as a barrier between irritants and the ocular surface.
If conservative therapy is not sufficient, a topical antihistamine, such as Zaditor® (ketotifen fumarate), can be used twice daily. Long-term safety studies have not been performed with this drug in dogs, however short-term use (less than 30 days) appears safe. Topical steroids can be utilized in the short-term but should be avoided as a maintenance therapy due to potential for corneal complications. If possible, surgery to correct any underlying conformation issues could be pursued.
Conjunctivitis can also be allergic in origin. In atopic dogs, conjunctivitis can be an early sign of a flare-up. Dogs can be affected unilaterally or bilaterally, although bilateral signs are more common. If only the eyes are involved, conservative therapy as described above could be instituted. Topical steroids can be prescribed to alleviate symptoms, but long-term use should be avoided. As an alternative, topical cyclosporine or tacrolimus are safer for long-term use and can be used twice or three times a day. In dogs with more generalized allergies (not just ocular signs), systemic therapy will often control ocular signs as well.
For more information about managing conjunctivitis in your patients, please do not hesitate to contact the University of Illinois ophthalmology service, either by phone or via our consult e-mail: vet-eyes@illinois.edu. Every effort is made to return consult calls and emails the same day or within 24 business hours.
By Katie Fleming, DVM, PhD, DACVO