Above: Dr. Tisha Harper is a clinical associate professor and the service head for small animal orthopedics and rehabilitation at the Veterinary Teaching Hospital.
Traumatic hip luxations are commonly seen in dogs and cats, with up to 83% of cases occurring secondary to vehicular trauma. Other causes of coxofemoral luxation include falls, spontaneous luxations, and unknown trauma. Bilateral luxations may also be seen. Although the hip may luxate ventrally and caudally, craniodorsal luxations are by far the most common direction of coxofemoral luxation, seen in approximately 80% of dogs and 73% of cats.
Anatomy
There are major and minor stabilizers of the coxofemoral joint. Major stabilizers of the hip are the joint capsule, ligament of the head of the femur, and the dorsal acetabular rim. Ancillary or minor stabilizers are the ventral acetabular ligament, gluteal muscles, hip adductors, and hip abductors.
For coxofemoral luxation to occur at least two of the major stabilizers need to be disrupted. Typically the joint capsule and ligament of the femoral head are disrupted. In severe cases the gluteal muscles may also be disrupted.
Clinical Examination
With craniodorsal luxation, the patient holds the limb in a characteristic manner, with adduction and external rotation of the limb. The stifle is typically rotated outward and the tarsus rotated inward. If the patient is placed on its back and the hind limbs extended caudally, the affected limb is shorter than the unaffected limb. With ventral luxation the opposite is true: the affected limb is longer than the unaffected limb and the patient carries the limb abducted and internally rotated. Patients with bilateral luxations are often unable to walk.
Abnormal positioning of the greater trochanter is also noted on examination of the patient. The orientation of the ilial wing, greater trochanter, and ischial tuberosity changes. There is an increased distance between the greater trochanter and the ischial tuberosity with craniodorsal luxation. You will also notice that a finger placed between the greater trochanter and the ischial tuberosity is not displaced if the femur is externally rotated. With ventral luxation there is medial displacement of the greater trochanter compared to normal and there is limited adduction and external rotation of the limb.
Manipulation and palpation of the limb will reveal pain, swelling, and crepitus over the coxofemoral joint. Palpation must be done gently to minimize damage to the articular cartilage of the femoral head.
Diagnosis
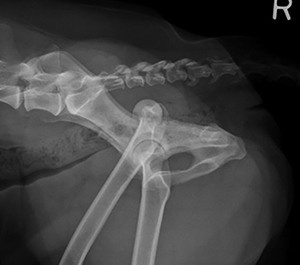
Diagnosis is confirmed on radiographs. Two orthogonal views must be taken. Radiographs must be taken not only to confirm the diagnosis of coxofemoral luxation but also to rule out other abnormalities that would preclude closed reduction of the luxation. These include fractures of the femoral head, neck, or greater trochanter or acetabular fractures. Avulsion fracture of the ligament of the head of the femur should also be ruled out. Pre-existing diseases that would prevent closed reduction include Perthes’ disease and hip dysplasia.
Treatment
Coxofemoral luxation can be treated by open or closed reduction. The aims of treatment are to reduce the luxation, stabilize the joint, and avoid further damage to the articular cartilage. The method of treatment is dictated by the direction of the luxation, the chronicity of the injury, the presence or absence of concurrent diseases (e.g., hip dysplasia), and whether there are concurrent injuries (e.g., polytrauma patients). Economic constraints may also dictate what procedure is ultimately chosen.
Closed Reduction
Never attempt a closed reduction without first taking radiographs!
Closed reduction requires the patient to be anesthetized as it is a painful procedure. Anesthesia will minimize muscle contractions that make closed reduction difficult. As vehicular trauma is the most common cause of coxofemoral luxation, ensure that the patient is stable before anesthetizing. Closed reduction should be attempted as soon as the patient is stable, however. This is important for the health of the articular cartilage and to prevent continued damage to the surrounding soft tissues. Closed reduction is most successful within the first 24 to 48 hours of trauma. After 4 to 5 days, closed reduction is difficult and often unsuccessful.
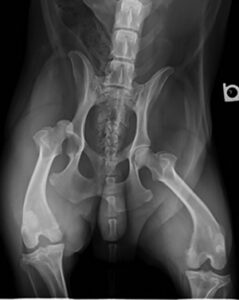
Place the patient in lateral recumbency with the affected limb uppermost. For patients that cannot have general anesthesia, sedation and an epidural should be considered. Countertraction of the pelvis is needed for closed reduction. Application of distal traction and external rotation will position the femoral head over the acetabulum, then internal rotation of the limb will seat the femoral head into the acetabulum (craniodorsal luxation). Assess limb length and the position of the greater trochanter to determine if reduction was successful.
When luxation occurs there is hemorrhage that eventually forms a blood clot in the acetabulum. The blood clot and fibrin, joint capsule, and remnants of the ligament of the femoral head sitting in the acetabulum must be displaced from the acetabulum to allow proper seating of the femoral head. It is therefore important to move the hip through a range of motion while pressing down on the greater trochanter to displace this material from the acetabulum. The hip should be moved through its range of motion for approximately 20 minutes.
Radiographs must again be taken to confirm that the hip has been reduced. The limb then needs to be placed in an Ehmer sling (craniodorsal luxation) or tape hobbles (ventral luxations) for 10 to 14 days to maintain the reduction. I prefer to place the sling before taking postreduction radiographs. The success rate following closed reduction is about 50%. If the joint reluxates easily, consider open reduction or a salvage procedure.
By Tisha Harper, DVM, MS, DipACVS-SA, DACVSMR, CCRP




