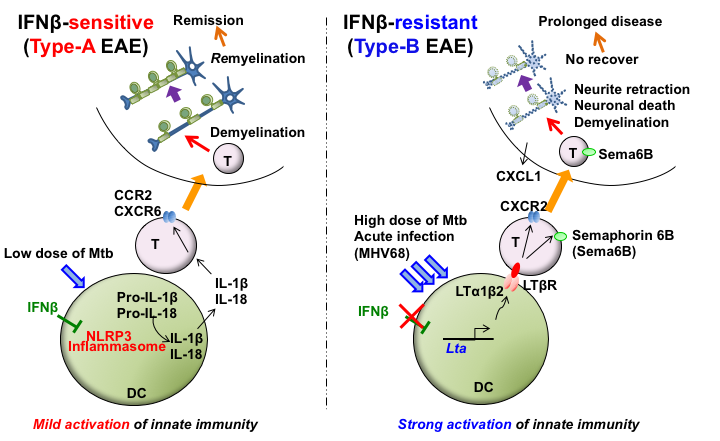
Mechanisms of IFN beta-sensitive and resistant EAERecently, we identified new drug candidates for multiple sclerosis (MS) patients who do not respond treatment of interferon β (IFNβ), which has been a first-line treatment to MS patients for over 15 years. The study was published in the journal Nature Neuroscience (Inoue et al., 2016; An interferon-β-resistant and NLRP3 inflammasome–independent subtype of EAE with neuronal damage). Using a mouse model of MS (EAE), we found that strong activation of innate immunity induced IFNβ-resistant EAE (termed Type-B EAE), whereas EAE induced by weak activation of innate immunity was sensitive to IFNβ treatment (termed Type-A EAE). While Type-A EAE required NLRP3 inflammasome (PNAS 2012, Sci. Signal. 2012), Type-B EAE did not. Instead, CXCR2 and LTβR, were central to the development of Type-B EAE (Nature Neuroscience 2016). We identified the molecular mechanism of Type-B EAE in detail. Importantly, relative expression of CXCR2 and LTBR genes were indeed enhanced in MS patients who did not respond to IFNβ therapy. Therefore, selective antagonist for these receptors may become alternative therapeutic drugs for MS patients who do not respond IFNβ therapy. In addition, evaluation of CXCR2 and LTBR expression levels may identify sensitivity of IFNβ therapy in MS patients. In this study, we also demonstrated that Type-B EAE showed neuronal damage in the CNS, a pathological hallmark of progressive form of MS. Therefore, Type-B EAE may be also reminiscent of a progressive MS, of which there is currently no therapeutic treatments. Because semaphorin 6B was central to the induction of neuronal damage in the Type-B EAE, inhibition of sempahorin 6B signaling may work for progressive MS patients.
This study was done at Duke University under Dr. Shinohara’s supervision.