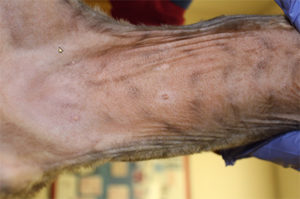
ABOVE: Figure 3. Hypotrichosis and erythema of ventral neck and thorax of a Basset Hound with Malassezia dermatitis secondary to allergic dermatitis.
Malassezia dermatitis is an inflammatory condition associated with increased numbers of Malassezia yeasts on the skin that lead to dermatitis and pruritus.
Predisposing factors for Malassezia proliferation and pathogenicity include increased environmental humidity and temperature, skin trauma, sebum quantity and quality, immune dysfunction, and genetic predispositions.
In dogs, Malassezia dermatitis is frequently associated with allergic dermatitis (e.g., environmental allergy, adverse food reaction, flea bite hypersensitivity); endocrinopathies, especially hypothyroidism; and other seborrheic conditions. In cats, Malassezia dermatitis has been associated with retroviral infections (i.e., feline immunodeficiency virus, feline leukemia virus), diabetes mellitus, neoplasia, and paraneoplastic syndromes.
Diagnosis
The diagnosis of Malassezia dermatitis is based on supportive clinical signs and cytology. The characteristic “footprint-shaped” yeast can be microscopically identified on cytologic exam of a skin lesion (Fig. 1, 2).
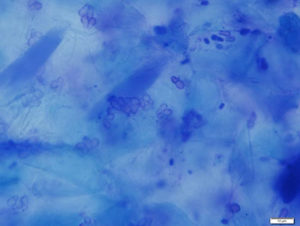
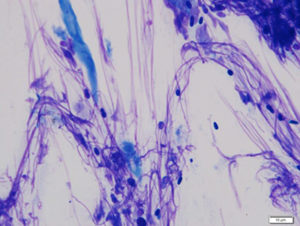
Sample collection technique is based on the location and type of skin lesions. Impression smears or swabs can be used for greasy lesions. Acetate tape preparations are ideal for drier lesions. Both swabs and acetate tape preparations are useful for body sites that are difficult to sample, such as skin folds and interdigital spaces.
For microscopic evaluation of the sample, utilize low power magnification to first identify cellular areas and then switch to oil immersion to identify and quantify the yeasts.
Malassezia spp. are commensal organisms, but if yeasts are identified on cytology from suggestive lesions, the infection should be addressed and treated. Some patients with Malassezia hypersensitivity can experience significant pruritus and erythema from a relatively small number of yeasts.
Clinical Signs
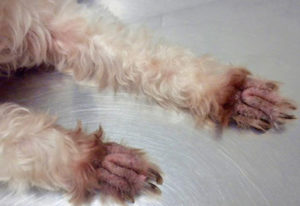
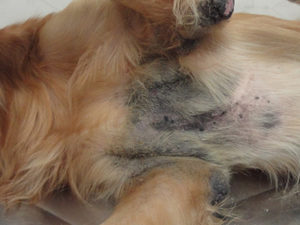
In dogs, Malassezia dermatitis lesions can be localized or generalized. They are typically characterized by erythema, scaling, and/or greasy exudation. In chronic cases, lichenification and hyperpigmentation also develop. Pruritus is often present and may lead to traumatic alopecia and excoriations. Paronychia (nail fold inflammation) may occur alone or in combination with more generalized pododermatitis. Brown discoloration of the adjacent claw and/or interdigital hair is often observed in cases of Malassezia paronychia (Fig. 3-5).
Malassezia is not considered a common pathogen in cats. The yeast dermatitis in cats is characterized by seborrhea oleosa, erythema, hypotrichosis, and the accumulation of greasy, adherent, brownish scales (Fig. 6). Sphynx and Devon Rex appear predisposed to Malassezia carriage, and often have a greasy exudate on the claws and in the claw folds. Pruritus can be present. Malassezia yeasts have also been associated with cases of facial dermatitis in Persian cats and chin acne. When Malassezia dermatitis is present in cats, consider an underlying cutaneous or systemic disease, such as allergies, endocrine and metabolic diseases, neoplasia, and infection with FeLV or FIV.
Treatment
Topical therapy can be used as the sole treatment for focal or generalized Malassezia dermatitis. Topical medication is important in cases with an incomplete or poor response to systemic treatment because of biofilm formation, and is also preferred in cases of yeast pododermatitis. Shampoos are typically applied once to twice weekly. Sprays, creams, lotions, or wipes are typically applied every 12 to 24 hours.
Various antifungal agents are marketed for the treatment of yeast skin infections. For both dogs and cats, these include topical azoles (e.g., miconazole, ketoconazole, clotrimazole, and climbazole), chlorhexidine preferentially in combination with azole agents for synergistic activity. Options just for dogs include selenium sulfide 1% to 2.5% and terbinafine.
For recurrent cases and patients with Malassezia hypersensitivity, a serologic and/or intradermal test may be performed and Malassezia antigen can be used in subcutaneous and sublingual allergen-specific immunotherapy for atopic dogs. Malassezia immunotherapy is not a replacement for topical or systemic antifungal therapies for the management of active Malassezia dermatitis. It may be considered in allergic patients with recurrent pruritic Malassezia dermatitis to reduce or prevent recurrences of Malassezia-associated dermatitis and pruritus.
Overall prognosis for Malassezia dermatitis is good. Prognosis is variable if the underlying cause of Malassezia dermatitis is not identified and/or managed successfully.
By Clarissa Souza, DVM, MSc, PhD

![[bassett with Malassezia dermatitis]](https://vetmed.illinois.edu/wp-content/uploads/2021/04/souza-fig-3.jpg)


